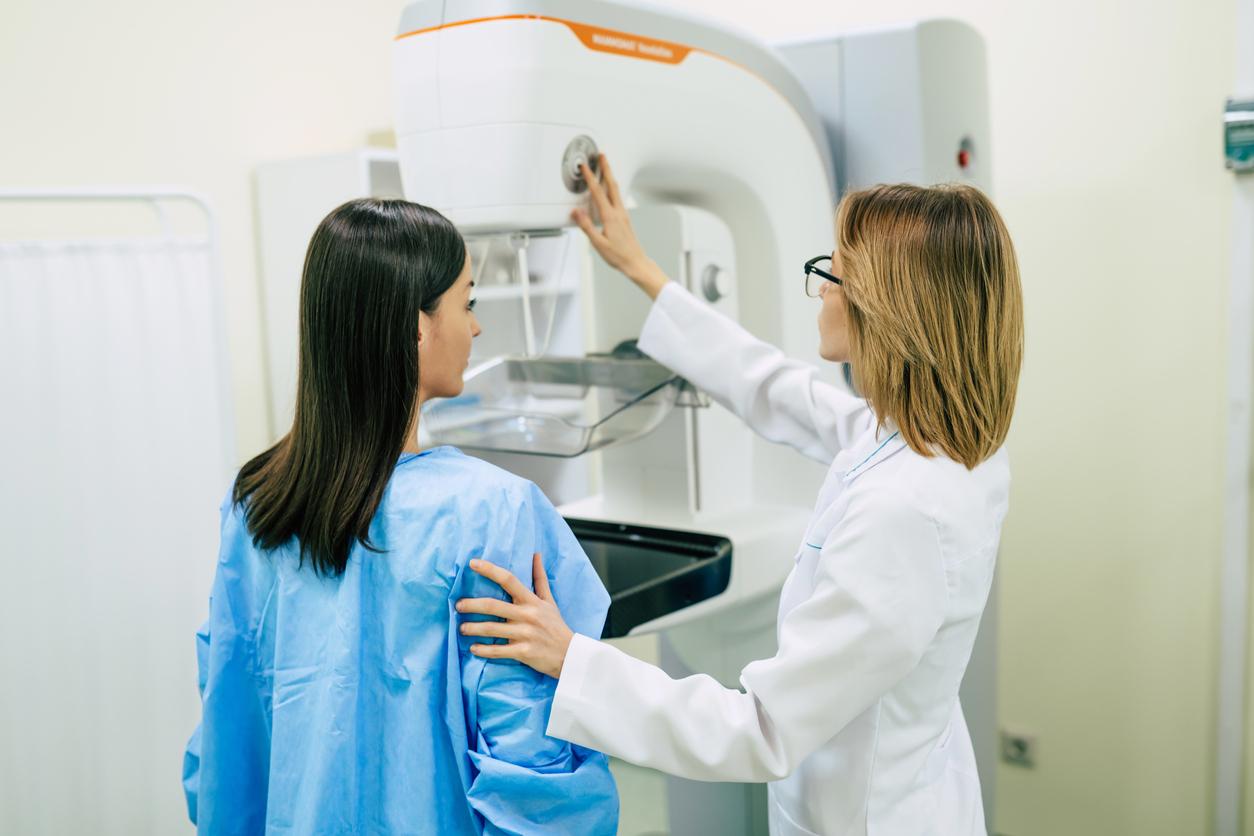
Study: More paid sick leave results in more cancer screenings
For most Americans, the two major obstacles to proper medical care are time and money. And while insurance can sometimes reduce healthcare costs, having time to visit the doctor is just as important.
Now, a new Tulane University study published in the New England Journal of Medicine has found that more people get screened for cancer when employers are mandated to provide paid sick leave. During a 7-year period covered by the study, breast cancer screening rates increased up to 4% and colorectal cancer screenings increased between 6-8% in areas exposed to policy-driven paid sick leave mandates.
“These non-monetary barriers to healthcare access matter,” said Kevin Callison, lead author and assistant professor of health policy and management at Tulane’s School of Public Health and Tropical Medicine and The Murphy Institute. “Improving or reducing these barriers can have meaningful impacts on people’s health.”
The U.S. is the only wealthy nation in the world to not federally mandate paid time off for being sick, according to the Center for Economic Policy and Research. According to the U.S. Bureau of Labor Statistics, about 1 in 4 American workers can’t take a single paid sick day.
The study, which was co-authored by researchers from Georgia State University and the University of California San Francisco, examined changes in breast cancer and colorectal cancer screening rates among 2 million private sector employees from 2012-2019, a time in which several states and cities adopted policies mandating paid sick leave. The workers were spread among 300 metropolitan statistical areas, 61 of which were exposed to a paid sick leave mandate during that timeframe.
Though the increases in screening rates may seem small, these results include workers who already had paid sick leave, meaning they were unlikely to decrease or increase cancer screening habits. If the results were scaled to focus only on workers gaining sick leave for the first time via mandates, Callison estimated that breast cancers screening rates increase 9-12% and colorectal screening rates increase 21-29%.
“Our effects become much larger if we're willing to assume that only the workers who are gaining paid sick leave coverage are the ones who are changing their screening behaviors,” Callison said.
Past studies have examined the relationship between sick days and cancer screening rates by comparing rates among those with leave to those without. But some workers are more health-conscious than others and may exclusively seek jobs that offer paid sick leave. By focusing on the change in screening rates brought by policy-driven mandates, this study removed some of the potential behavior-based biases.
“Because we focused on these policies that drive changes in coverage rather than people self-selecting into coverage, our argument is that we have a more accurate estimate of the relationship between paid sick leave and cancer screening,” Callison said.
The results underscore the value of sick days. Callison said it’s “reasonable to assume that more cancer screenings lead to earlier detection and better outcomes,” but more research is needed to determine if paid sick leave means cancers are caught earlier and if mortality rates decline.
To Callison, these results also represent one potential way of increasing healthcare equity in the United States.
The majority of those without paid sick leave are people of color and those with less wealth and less education. And though 17 states and 18 cities have adopted paid sick leave, 18 states have passed laws prohibiting cities from passing similar mandates.
“We know that racial and ethnic minorities tend to have higher mortality rates for certain cancers,” Callison said. “So are things like this going to improve those gaps? That’s really the next step where we want to go.”